Head and Neck Fellowship
The Vanderbilt Head and Neck, Cranial Base and Microvascular Reconstructive Surgery Fellowship is an outstanding one-year clinical position within the department of Otolaryngology Head and Neck Surgery. There are two positions available per year, beginning in July. This fellowship is offered through the American Head & Neck Society Match and is AHNS-accredited.
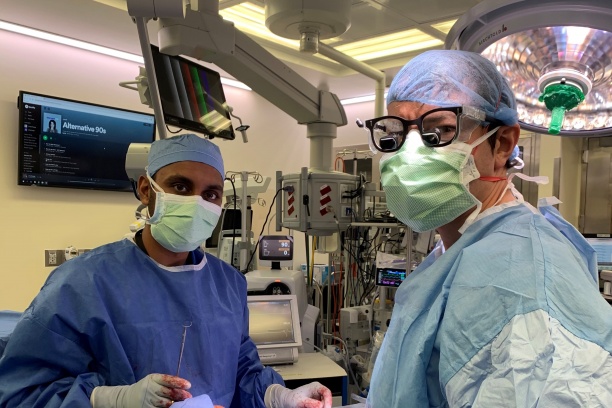
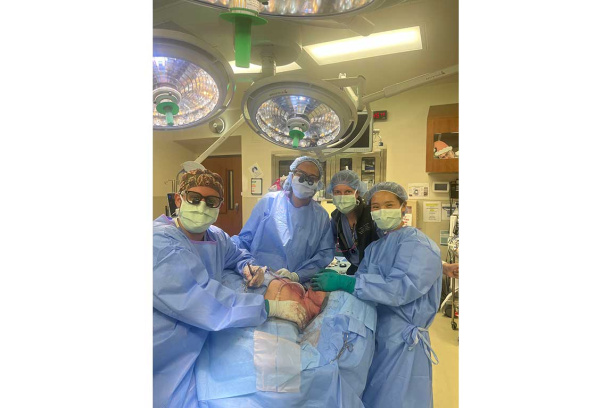
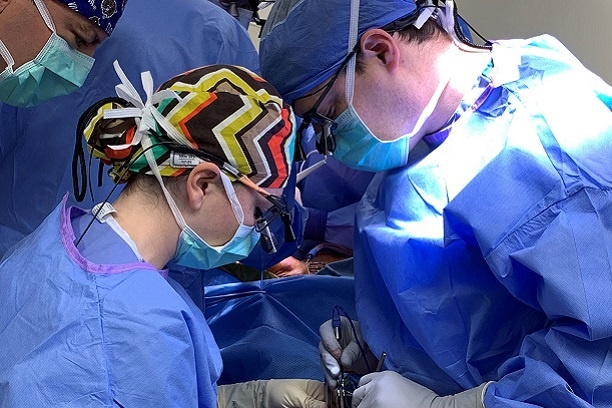
The fellowship provides broad based exposure to head and neck oncologic surgery and reconstructive surgery. The fellows participate in a high volume of mucosal, salivary, endocrine, cutaneous and skull base tumor treatment as well as a significant involvement in the treatment of paragangliomas and lesions of the parapharyngeal space. Comprehensive training in locoregional and free flap reconstruction completes the preparation of our fellows for their future practices.
Fellows are clinical instructors at Vanderbilt University School of Medicine, giving them experience and leadership in the academic setting. They are given surgical privileges at Vanderbilt University Medical Center, Monroe Carell Jr. Children's Hospital at Vanderbilt and the VA Hospital. There are ample opportunities for research within the head and neck division and excellent mentorship from faculty with multiple different focuses and career paths.
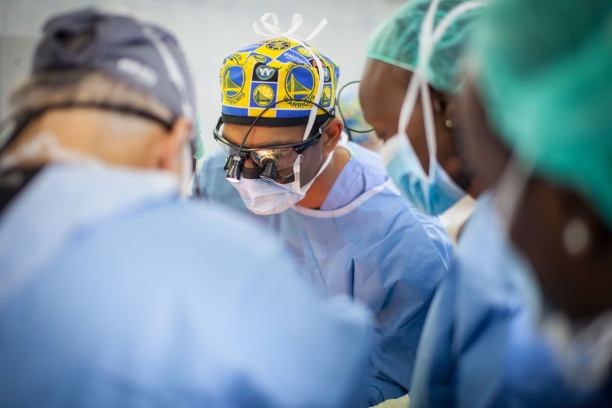
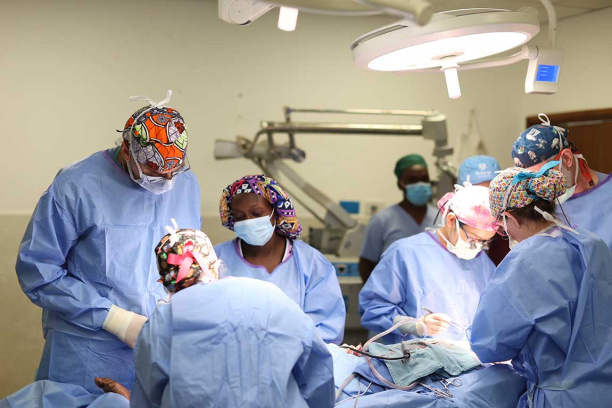
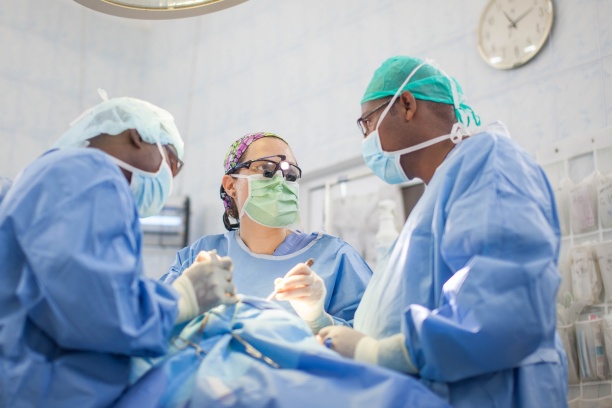
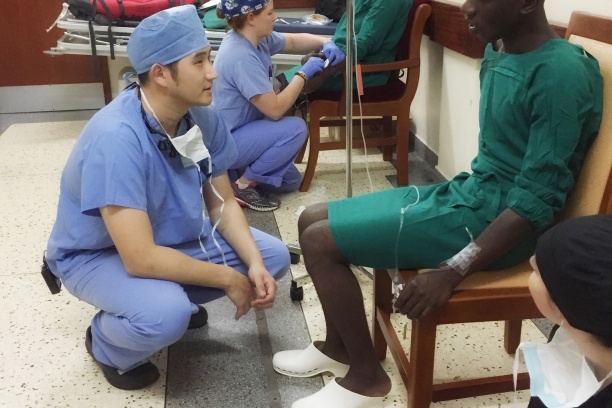
Fellows in the Vanderbilt Head and Neck, Cranial Base and Microvascular Reconstructive Surgery program also have the opportunity to participate in multiple global outreach programs primarily to Africa. During these trips, fellows utilize their medical and leadership skills by treating patients and training local physicians in head and neck surgical techniques.
-
Our overriding goal is to build upon the skills learned in residency and provide the necessary technical, clinical, instructional and administrative skills to prepare our trainees to begin a career as a head and neck oncologic and reconstructive surgeon. This includes all aspects of the clinical care of head and neck patients, as well as the teaching, research and administrative skills expected in an academic surgeon.
-
- Competency in oncologic resection of head and neck tumors in all sites
- Competency in the workup and treatment of thyroid and parathyroid neoplasms, including ultrasound and guided biopsy proficiency
- Competency in the reconstruction of all major bony and soft tissue defects in the head and neck
- Competency in transoral robotic surgery
- Integration into a multidisciplinary team in the care of head and neck patients
- Development of teaching skills and resident training in and out of the operating room
- Preparation for applying and securing a position as a head and neck surgeon
-
Candidates must complete a residency in Otolaryngology, and be board certified or board eligible.
Additionally, fellows must be able to:
- obtain an unrestricted Tennessee Medical License. At least one year of training in an AMA accredited program in the United States is required for International MD licensure in the state of Tennessee. Requirements for Tennessee Full Medical Licensure are available from the TN Board of Medical Examiners.
- obtain a Tennessee DEA. Information on requirements for DEA registration are available from the US DEA.
- and provide proof of citizenship or Visa status (if applicable). Visa information (if applicable) should be provided with the application. Please note all of the requirements and be advised that we do not sponsor visas for fellows. The visa you would need to independently acquire must permit you to work and may not be a student visa as this position requires teaching. For Visa information, please consult the US State Department website.
- Apply through the American Head and Neck Society.
-
Clinical duties: The two fellows rotate between the faculty members in alternating 6-week rotations with significant crossover based on the clinical activities at any given time. The fellows provide their planned weekly schedule to the team (faculty and residents) each week with dedicated OR and clinic time. Robotic surgery is stressed in one of these two blocks to provide a more focused experience while the rest of the breadth of extirpative and reconstructive procedures are balanced between the two rotations. In these alternating 6-week blocks, one fellow spends a full day each Monday at the adjacent VA medical center both in the OR and in the clinic treating and evaluating head and neck patients.
While the fellows carry an instructor level position at the medical center, the focus is to work with the head and neck faculty. The fellows own cases are a small portion of the experience and originate from ER and inpatient consults. Each fellow covers attending level call roughly every 6th weekend and one holiday per year.
Each fellow is expected to spend multiple clinic sessions each year with our head and neck medical and radiation oncologists
Academic duties:
- Serve as an active instructor to the residents during operative cases, clinic and rounds
- Attend weekly multidisciplinary tumor board (optional weekly tumor boards for melanoma/cutaneous malignancies, endocrine, etc. also available)
- Attend Monthly head and neck research meeting
- Encouraged to attend monthly head and neck division meetings
- Attendance at national meetings is encouraged
- The fellows are expected to attend a microvascular reconstruction course and TORS course if they are granted admission
- Weekly clinical case conference run by the fellows focused on the AHNS fellowship curriculum with at least one article cited for discussion each week
- One off-hours educational meeting during each 10-week resident rotation organized by the fellows (Journal club, ultrasound training, etc.)
- While there is not a specific research criterium for completing the fellowship, each fellow is expected to participate in novel or ongoing research projects within the division
-
Vanderbilt Head and Neck Surgery fellows become leaders in the field, both in academic and clinical settings. Of the head and neck oncologic fellows we have trained so far, 45 are in university-based academic practice, and at least 23 are in leadership positions, including two Cancer Center Directors, six Chairs, a dozen Head & Neck Surgery Division Chiefs, and three Program Directors. ·
- 2027 – Haley Mann – Incoming Fellow
- 2027 - Andrew Prince – Incoming Fellow
- 2026 – Cassie Pan – Current Fellow
- 2026 – Annie Moroco – Current Fellow
- ·2025 – Vivian Zhu – Assistant Professor - University of Louisville Medical Center, Louisville, KY
- 2025 – David Zimmer - Assistant Professor – University of Louisville Medical Center, Louisville, KY
- 2024 – Pratyusha Yalamanchi- Assistant Professor – University of Michigan Medical Center, Ann Arbor, MI.
- 2024 – Ramez Philips – Assistant Professor – Thomas Jefferson University, Philadelphia, PA.
- 2023 – Melanie Hicks – Private Practice – ENT Specialty Care of MN, Maple Grove, MN.
- 2023 – Andrew Katz – Assistant Professor, Cambridge Health Alliance, Cambridge, MA.
- 2022 – Chen Lin, MD – Assistant Professor, University of Chicago, Chicago, IL.
- 2022 – Dan Sharbel, MD – Assistant Professor, medical College of Georgia, Augusta, GA.
- 2021 – Kevin John Kovatch, MD – Assistant Professor, University of Connecticut, Farmington, CT.
- 2021 – Catherine Alessandra Colaianni, MD – Assistant Professor, University of North Carolina, Chapel Hill, NC.
- 2020 – William A. Stokes III, MD – Assistant Professor, Rochester Regional Health, Rochester, NY.
- 2020 – Sarah Michelle Drejet, MD – Assistant Professor, Department of Otolaryngology, University of Utah, Salt Lake City, UT.
- 2019 – Nolan Seim, MD – Assistant Professor of Head and Neck Surgery, Department of Otolaryngology, Ohio State University, Columbus, OH.
- 2019 – Brian P. Cervenka, MD – Assistant Professor, University of Colorado, Aurora, CO.
- 2018 – Jo-Lawrence Bigcas, MD – Assistant Professor, Head and Neck Surgery, University of Nevada Las Vegas, Las Vegas, NV.
- 2018 – Justin Bond, MD, FACS – Assistant Professor, Head and Neck Surgery, University of Kansas, Kansas City, KS.
- 2017 – Alice Tang, MD – Assistant Professor, Head and Neck & Endocrine Surgery, University of Cincinnati, Cincinnati, OH.
- 2017 – Shethal Bearelly, MD – Assistant Professor, Head and Neck Surgery, The University of Arizona, Tucson, AZ.
- 2016 – Michael Sim, MD – Assistant Professor, Head and Neck Surgery, Indiana University School of Medicine, Indianapolis, IN.
- 2016 – Sunshine Dwojak, MD, MPH – Physician, Kaiser Permanente; Clackamas, OR.
- 2015 – John Heaphy, MD – Physician, King Faisal Specialist Hospital and Research Center – Jeddah, Jeddah, Saudi Arabi.
- 2015 – Kelly Groom, MD – Physician, Head and Neck Surgery, Triple Army Medical Center; Honolulu, HI
- 2014 – Christopher Fundakowski, MD – Professor, Head and Neck Surgery, Jefferson University, Philadelphia, PA.
- 2014 – Eric Wirtz, MD – Chief, Head and Neck Surgery, Tripler Army Medical Center, Honolulu, HI.
- 2013 – Adam J. Luginbuhl, MD –Professor; Thomas Jefferson University Hospital, Department of Otolaryngology – Head and Neck Surgery, Philadelphia, PA.
- 2013 – Benjamin Johnston, MD – Assistant Professor, Vanderbilt Medical Group Franklin – Ear Nose and Throat, Franklin, TN.
- 2012 – Clinton “Casey” Kuwada, MD – Physician, co-director of the Head and Neck Cancer Program at Hartford Hospital’s Helen & Harry Gray Cancer Center; Wethersfield, CT.
- 2012 – Christian Hasney, MD, FACS – Associate Professor, Head and Neck Surgical Oncology, Tulane University; Site Director, Ochsner Medical Center, New Orleans, LA.
- 2011 – Alexander Langerman, MD –Professor, Head and Neck Surgery, Vanderbilt University Medical Center, Nashville, TN.
- 2011 – Kelly Cunningham, MD – Physician, Head and Neck Surgery, Carle Foundation Hospital, Urbana, IL.
- 2010 – Ronald Walker, MD – Associate Professor, Department of Otolaryngology – Head & Neck Surgery, St. Louis University Health Sciences Center, St. Louis, MO.
- 2010 – Sarah Rohde, MD, MMHC –Chief, Division of Head and Neck Surgical Oncology; Associate Professor, Department of Otolaryngology – Head and Neck Surgery, Vanderbilt University Medical Center, Nashville, TN.
- 2009 – Matthew Old, MD – Department Chaorman; University of Washington, Seattle, WA.
- 2009 – Freedom Johnson, MD – Private Practice, Blue Ridge ENT & Allergy, Morganton, NC.
- 2008 – Nadir Ahmad, MD – Division Head, Otolaryngology–Head & Neck Surgery, Cooper University Hospital, Camden, NJ; Associate Program Director, Otolaryngology–Head & Neck Surgery Residency, Cooper University Hospital; Director, Head & Neck Cancer Program, MD Anderson at Cooper Cancer Center; Professor, Cooper Medical School of Rowan University; Adjunct Associate Professor, University of Texas, MD Anderson.
- 2008 – Kyle Mannion, MD, FACS – Associate Professor, Department of Otolaryngology, Vanderbilt University Medical Center, Nashville, TN.
- 2007 – Francis Ruggiero, MD – Director of Head and Neck Surgery, Penn State Milton S. Hershey Medical Center, Hershey, PA.
- 2007 – Chad Zender, MD, FACS – Professor of Otolaryngology and Associate Chief Medical Officer, University of Cincinnati College of Medicine; Center of Excellence Co-Leader for Head and Neck Cancer, UC Cancer Institute, UC Health, Cincinnati, OH.
- 2006 – Becky Massey, MD – Associate Professor, Head and Neck Surgery, Medical College of Wisconsin, Milwaukee, WI.
- 2006 – Jason Hunt, MD, FACS – Clinical Director, Head and Neck Surgical Oncology, Huntsman Cancer Hospital; Professor, University of Utah, Salt Lake City, UT.
- 2005 – Cecelia Schmalbach, MD – David Myers, MD Professor and Chair, Department of Otolaryngology – Head & Neck Surgery, Lewis Katz School of Medicine, Temple University; Director, Temple Head & Neck Institute, Philadelphia, PA.
- 2005 – Scharu061206kh Jalisi, MD – Chief of Otolaryngology, Beth Israel Medical Center, Boston, MA.
- 2004 – George Coppit, MD – Director of Head and Neck Surgery, Walter Reed Army Medical Center, Washington, D.C.
- 2004 – Derrick Lin, MD, FACS – Daniel Miller Professor and Associate Chair of Otolaryngology–Head and Neck Surgery; Director, Division of Head and Neck Surgery, Massachusetts Eye & Ear Infirmary, Harvard Medical Center, Boston, MA.
- 2003 – Paul Van der Sloot, MD – Private Practice, Denver, CO
- 2003 – Robert Lorenz, MD – Surgeon, Head and Neck Surgery Section, Head & Neck Institute; Medical Director of Payment Reform, Risk & Contracting, Cleveland Clinic, Cleveland, OH.
- 2002 – William P. Magdycz, MD – Director of Head & Neck Surgery, Portsmith Naval Medical Center, Portsmith, VA; Carilion Roanoke Memorial Hospital, Roanoke, VA.
- 2002 – Terry Johnson, MD – Chairman, Otolaryngology – Head & Neck Surgery, Naval Medical Center, San Diego, CA.
- 2002 – Peter Hunt, MD, FACS – Private Practice, Associates in ENT; Director, Head and Neck/Melanoma Center of Excellence, Memorial Cancer Institute; Attending, Chattanooga Tumor Clinic, Chattanooga, TN.
- 2001 – Garth Olson, MD – Professor, Director of Head & Neck Surgery, University of New Mexico, Albuquerque, NM.
- 2001 – Mumtaz Khan, MD, FACS – Professor, Chair of Otolaryngology, Surgical Subspecialties Institute, Cleveland Clinic Abu Dhabi, Abu Dhabi, UAE.
- 2000 – Alain Sabri, MD, MDH, FACS – Professor, Founding Chair, Department of Otolaryngology–Head and Neck Surgery; Dean, Gilbert and Rose-Marie Chagoury School of Medicine, Lebanese American University, Beirut, Lebanon.
- 2000 – Joseph C. Sniezek, MD, MBA, FACS – Medical Director of Head & Neck Endocrine Surgery, Swedish Medical Center, Seattle, WA.
- 1999 – Chris Sullivan, MD – Professor, Head & amp; Neck Surgery, Wake Forest University Baptist Medical Center, Winston-Salem, NC.
- 1998 – Frank Miller, MD, FACS – Professor and Chairman; Thomas Walthall Folbre, M.D. Endowed Chair in Otolaryngology; Director, Head and Neck Surgery, UT Health San Antonio, San Antonio, TX.
- 1997 – Theodoros N. Teknos, MD – Clinical Professor, Department of Otolaryngology, School of Medicine; Deputy Director for University Hospitals, Case ComprehensiveCancer Center; President, University Hospitals Seidman Cancer Center, Cleveland, OH.
- 1996 – Don Weed, MD, FACS – Professor; Co-Leader, Head and Neck Site Disease Group; President Medical Staff, University of Miami Hospital and Clinics, University of Miami, Miami, FL.
- 1995 – Robert J. Sinard, MD, FACS –Professor & Department of Otolaryngology–Head and Neck Surgery, Vanderbilt University Medical Center, Nashville, TN.
- 1994 – William B. Armstrong, MD – Professor, Chairman, Department of Otolaryngology–Head and Neck Surgery, University of California Irvine, Irvine, CA.
- 1993 – John Wanamaker, MD – Associate Professor, Department of Otolaryngology, Washington DC VA Medical Center, Washington, DC.
- 1992 – Frank Civantos, MD, FACS – Professor and Director of Head & Neck Surgery, University of Miami, Miami, FL.
- 1991 – John Coniglio, MD – Clinical Associate Professor, Rochester Regional Health, Rochester, NY.