Glaucoma is an optic neuropathy which causes irreversible vision loss and blindness due to degeneration and death of retinal ganglion cells (RGCs). Although high intraocular pressure (IOP) is a known risk factor, some patients with normal IOP develop glaucoma. The overall aims of our research are to improve mechanistic understanding of IOP regulation and RGC degeneration in the context of elevated and normal IOP.
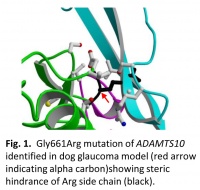
Previously, we identified a mutation in a microfibril-associated gene, ADAMTS10, in a dog model of primary open-angle glaucoma (fig. 1). This led us to form the microfibril hypothesis of glaucoma, which in general states that defective microfibrils may be an underlying cause of glaucoma. Microfibril defects could contribute to glaucoma through alterations in biomechanical properties of tissue and/or through effects on signaling through TGFβ, which is well established to be elevated in the aqueous humor of glaucoma patients.
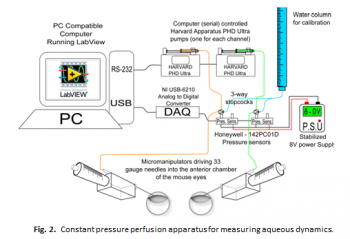
Currently we are studying two mouse lines with defective microfibrils that develop glaucoma without elevated IOP. Mouse IOP is measured by rebound tonography and aqueous humor dynamics are characterized using a constant pressure perfusion apparatus (fig. 2).
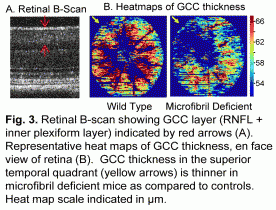
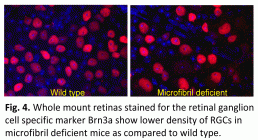
Glaucomatous RGC loss is determined by spectral domain optical coherence tomography (SD-OCT) to follow retinal nerve fiber layer thickness (fig. 3) and by immunocytochemistry of retinal whole mounts (fig. 4).
A translational focus in our lab is the investigation the effectiveness of sartan drugs in preventing or slowing the progression of glaucoma. Sartans, such as losartan, are angiotensin II receptor antagonists commonly used to treat systemic hypertension. Recently, sartans have been shown to be an effective treatment for Marfan syndrome, a disease caused by microfibril deficiencies. For these studies, we are carrying out retrospective cohort studies of glaucoma patients to determine if sartans protect against initial development of glaucoma or slow progression of visual field loss for those previously diagnosed. In addition, we are testing the efficacy of losartan in prevention and treatment of glaucoma in our normal tension mouse models and in experimental glaucoma induced by injection of microbeads into the anterior chamber.
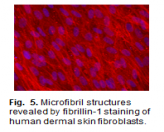
Following up on our identification of ADAMTS10 in a dog glaucoma model, we are also currently developing Adamts10 knockout mice and human cell lines using CRISPR technology. Aqueous humor dynamics and RGC loss will be characterized in Adamts10-/- mice and formation of microfibrils (fig. 5) will be studied in Adamts10-/- cell lines.
Publications