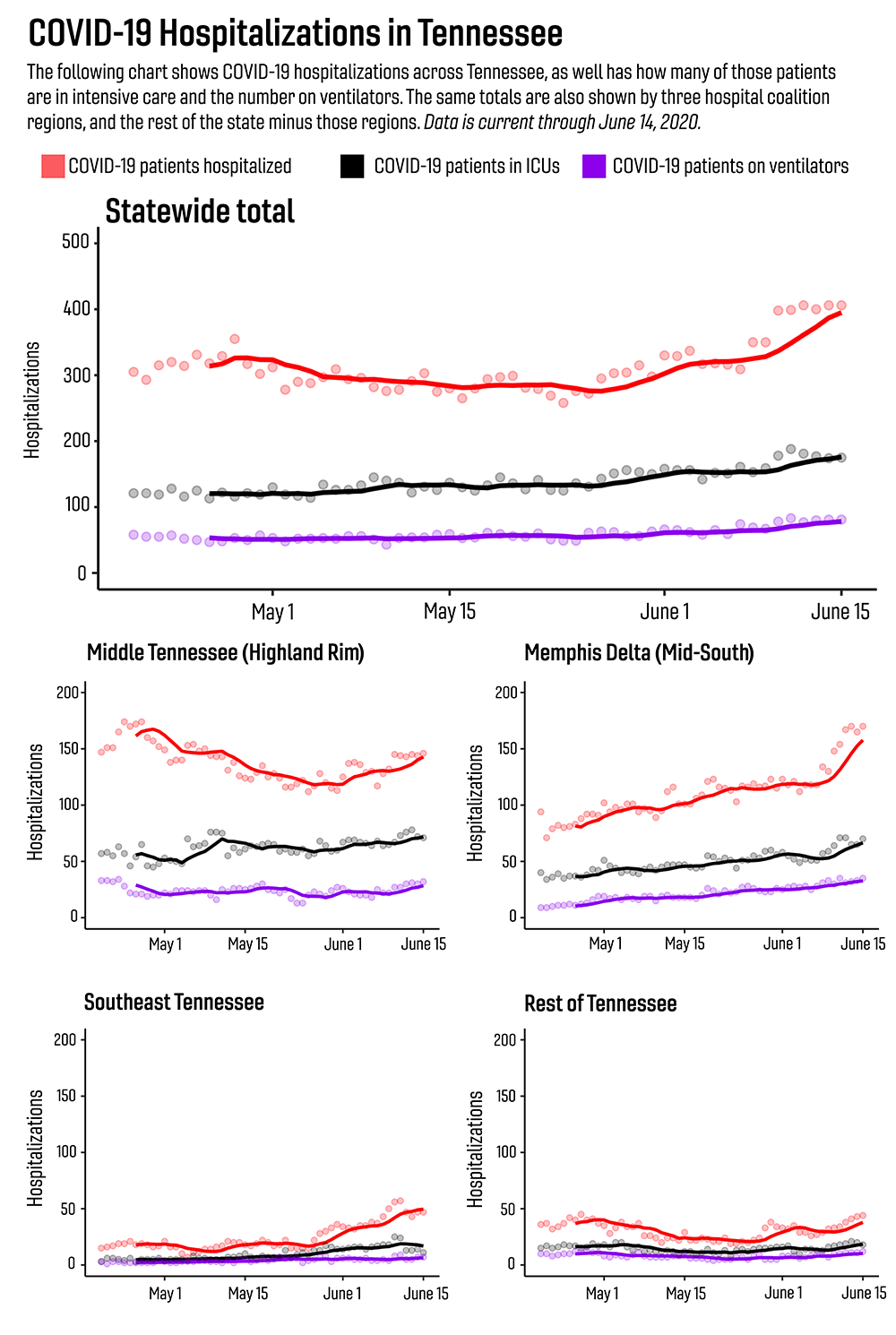
The number of hospitalized COVID-19 patients reached its highest level to date on June 15, when more than 400 patients were hospitalized across Tennessee, according to a report from researchers at Vanderbilt University Medical Center and Vanderbilt University School of Medicine.
The researchers stress that with few exceptions, the rise in COVID-19 hospitalizations has not yet put acute strain on the Tennessee hospital system — but a recent rise in cases, coupled with new modeling of hospitalizations, highlights that the situation must be closely tracked moving forward.
Most COVID-19 patients were hospitalized in Middle Tennessee, the Memphis Delta region and Southeast Tennessee around Chattanooga. The largest increases were in the Memphis Delta region and Southeast Tennessee around Chattanooga.
“The recent rise in hospitalizations is not a simple story, and is a story with multiple parts,” said John Graves, PhD, associate professor of Health Policy and director of the Center for Health Economic Modeling at Vanderbilt. “The rise in hospitalizations is as much about the virus expanding its footprint into additional areas of the state as it is about hospitalizations increasing in facilities that were already treating COVID-19 patients.
“And as hospitals see a welcome return of patients for elective procedures, it creates a thinner cushion to absorb a sudden and unexpected rise in COVID hospitalizations. It’s a situation that bears watching very closely.”
The rise in hospitalizations has increased as the number of positive cases has grown but has not yet put stress on the state’s hospital system, Graves added. Tennessee has not yet seen the surge in hospitalizations that has been seen in some neighboring states.
To explain this, Graves and fellow researchers, Melinda Buntin, PhD, Mike Curb Professor of Health Policy and chair of the Department of Health Policy, and Melissa McPheeters, PhD, research professor and co-director of the Center for Improving the Public’s Health Through Informatics, developed a case mix index (CMI) to calculate the risk profile of COVID-19 patients across the state using data from the Centers for Disease Control and Prevention on a primary risk factor, age.
The analysis shows that while the number of cases are growing, the growth is primarily in younger populations, which the CDC and other research have generally shown to have a lower likelihood of requiring hospitalization. When more cases occur in more vulnerable populations, such as the elderly and those with underlying health conditions, hospitalizations are more likely to spike.
But even as cases continue to increase so will hospitalizations, even if they represent a small proportion of total cases. If current transmission trends continue, the state may reach 1,000 concurrent hospitalizations in late July or early August, the team reported.
“As we have since the epidemic began, we are continuing to heavily stress that Tennesseans need to keep doing what they did early on, and that is to be very vigilant about social distancing, be consistent with hand hygiene and do your part to slow the spread,” McPheeters said. “It will be imperative to have a strong public health response in the form of widespread testing, effective contact tracing and recommendations for isolation of cases as we move forward.”