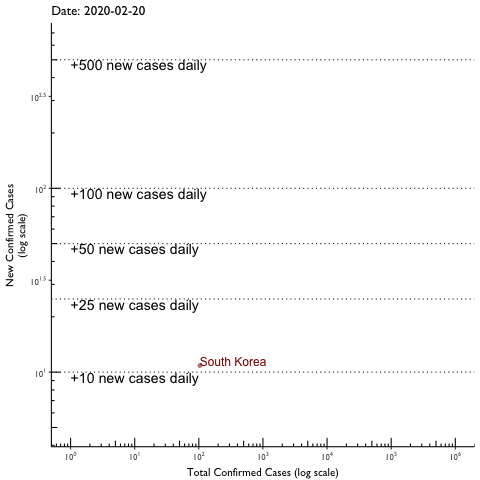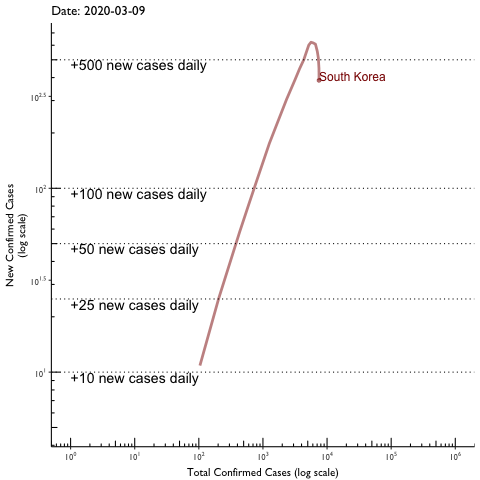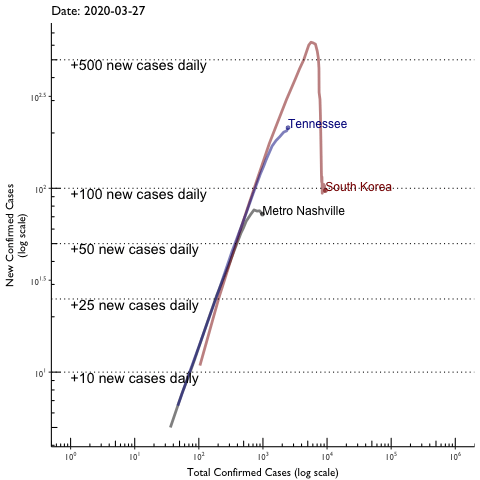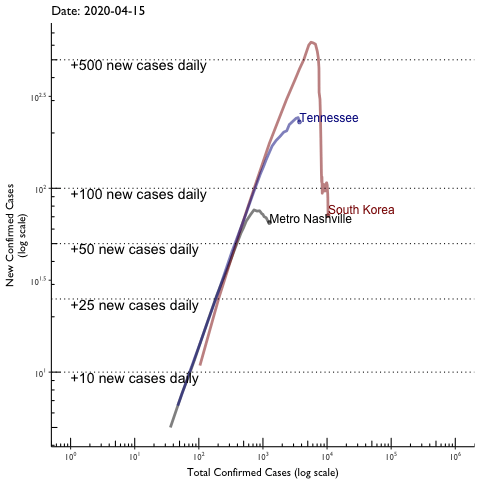
Vanderbilt University Medical Center researchers have found evidence of the rate of COVID-19 infection slowing in Tennessee, which reduces the chance that the state will run out of hospital capacity for patients.
They stress, however, that social distancing is needed to keep the rate of spread low and that any future rollback of social distancing policies must be contingent on widely available testing and comprehensive tracing of infected patients and the people they were in contact with.
“We all want to go back to some sort of normal, but to be able to relax some of the social distancing guidelines, you have to have in place widespread testing and robust contact tracing,” said John Graves, PhD, associate professor of health policy and director of the new Center for Health Economic Modeling at Vanderbilt.
The model uses daily updates from the Tennessee Department of Health data to adjust projections quickly.
“These unique advantages allow us to make more tailored predictions for our state because of our state-specific data sources, especially as we continue to feed new data into the model,” said Graves.
The model predicts if the current social distancing policies continue to reduce the spread of the disease, there would be an estimated peak of hospitalizations in mid-June. If the state were to experience additional gains from social distancing, under that more optimistic scenario the peak of hospitalizations could be lower and could be as early as mid-May.
Maintaining the current rate of spread of the virus, or with additional gains that reduce that rate of spread, would also prevent hospitals in the state from being overwhelmed, the model indicates. With approximately 10,000 staffed beds in the state, many of which are occupied by other types of patients, the “status quo” scenario estimates about 5,000 hospitalizations.
If the state were to prematurely lift current social distancing policies and guidelines, it would almost certainly cause hospitals to be overwhelmed and cause the peak of transmission to be later in the summer or after, according to the model.
Other modeling has suggested different outcomes and scenarios in Tennessee, but the Vanderbilt model is calibrated specifically to Tennessee and becomes further calibrated and refined as more data becomes available.
“Our model will change often as new data are available and we learn more about the spread of the virus,” said Graves.
The model was shared this week with public health officials and policy makers at the state and local levels. The model will continue to be refined and will produce regional models and more finely tuned pictures of what’s happening throughout Tennessee in the coming days.
The modeling team also includes Shawn Garbett, MS, an assistant in the VUMC Department of Biostatistics, Melissa McPheeters, PhD, research professor in the Department of Health Policy and co-director of the Center for Improving the Public’s Health Through Informatics, Melinda Buntin, PhD, Mike Curb Professor of Health Policy and Chair, Department of Health Policy, and Peter Rebeiro, MD, assistant professor of medicine at VUMC, and receives input from Vanderbilt’s Health Policy and Public Health Advisory Panel.