To share on Twitter, click the button below or credit @VI4research!
Sharing elsewhere? Credit this page.
Click here for a printer friendly version!
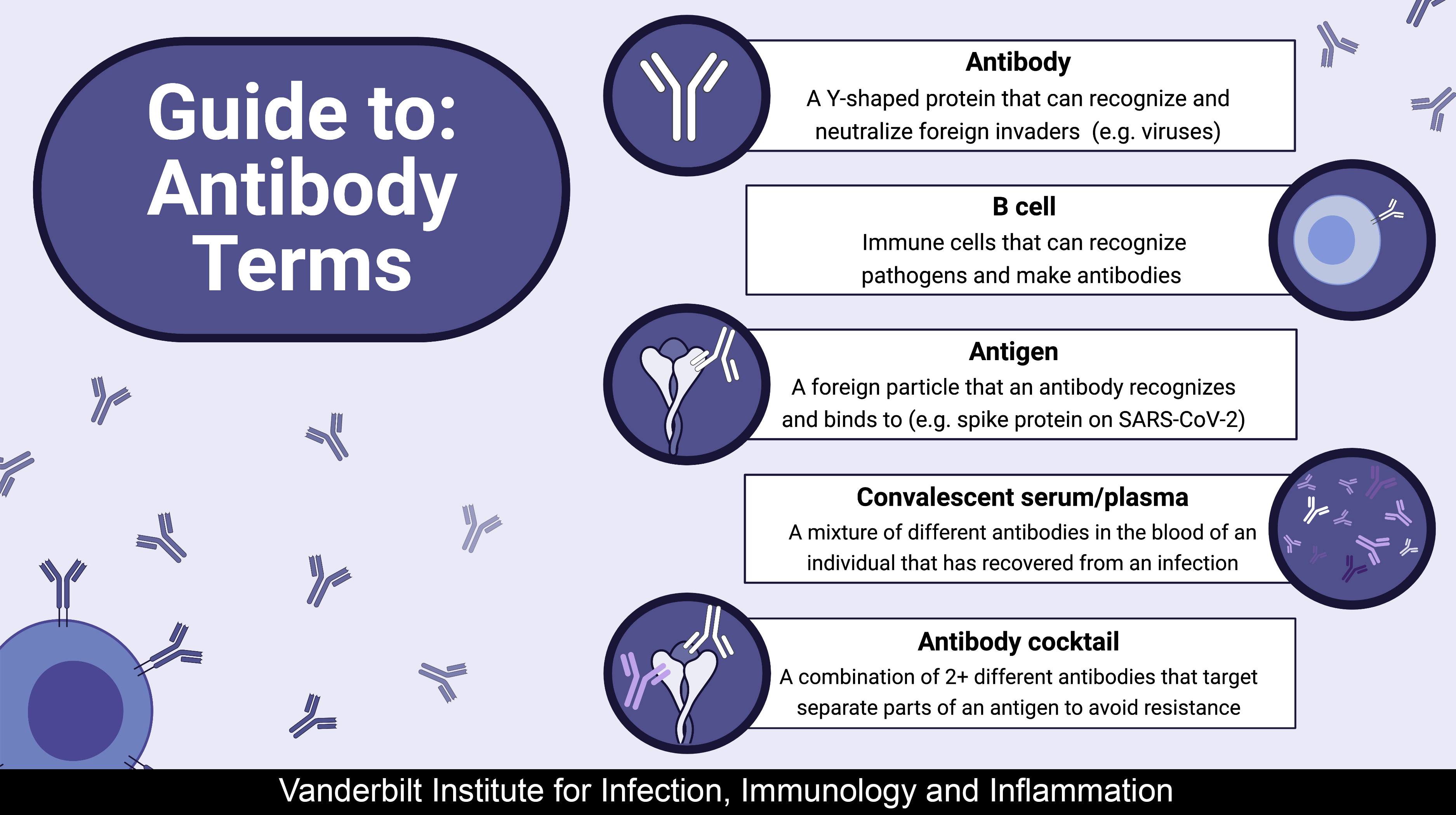
Guide to: Antibody Terms
Antibodies and B cell
Most of the vaccines that protect us from viruses do so by stimulating your body to produce antibodies. Antibodies are y-shaped proteins that circulate in the blood and recognize and fight off pathogens such as viruses. Immune cells called B cells recognize the pathogens and make a range of antibodies in response to an infection. Since B cells mix and match the genes that code for antibodies, there are theoretically 1017 different combinations of genes. This process allows for a tailored response for any pathogen we encounter and is how your immune system can neutralize the numerous pathogens it faces over your lifetime. As an infection persists, B cells can try out different antibodies, sequentially honing themselves to most effectively fight off the virus.
Antigens
If vaccines are like a training camp for your B cells, antigens (typically proteins) are the target practice. B cells practice their defenses against a harmless antigen (like in a vaccine) so that when the real virus comes along, they can immediately start making the most useful antibodies to fight the virus. Vaccines rely on producing the best antigens to train and build the most effective immune response. COVID-19 vaccines use the spike protein that is on the virus’s surface as an antigen to elicit antibodies. Antigen tests, also referred to as ‘rapid’ testing, detect SARS-CoV-2 proteins in your saliva and are also essential diagnostics for SARS-CoV-2 infection.
Convalescent serum/plasma and antibody cocktail
There are a few different types of antibody-based therapeutics. Convalescent serum/plasma is isolated from the blood of patients that have recovered from infectious diseases, such as COVID-19, and it contains all of the antibodies currently circulating in the body. Virus-specific antibodies will make up a large portion of serum after infection and can be given directly to other patients to provide some immunity to viruses such as SARS-CoV-2. However, since the total serum dilutes the most effective SARS-CoV-2 antibodies, this hasn’t proven to be a very effective strategy for COVID-19 treatment (this has worked with other infectious diseases, though). We can also isolate the most effective antibodies from the blood and use them as a single antibody (called a monoclonal antibody) or as a combination of two or more antibodies (called an antibody cocktail). Cocktails can be advantageous in the case of rapidly evolving pathogens. Emerging SARS-CoV-2 variants have modified versions of the spike protein – and our antibodies may not recognize them anymore. It may be easy for a virus to evolve changes in a portion of itself to escape an antibody. However, it is more difficult to evolve simultaneously in multiple areas to avoid both antibodies in a cocktail as they target separate parts of an antigen. Numerous antibody cocktails have received emergency use authorization from the FDA to treat COVID-19, and others are in late-stage clinical trials.
Graphics were created using BioRender.